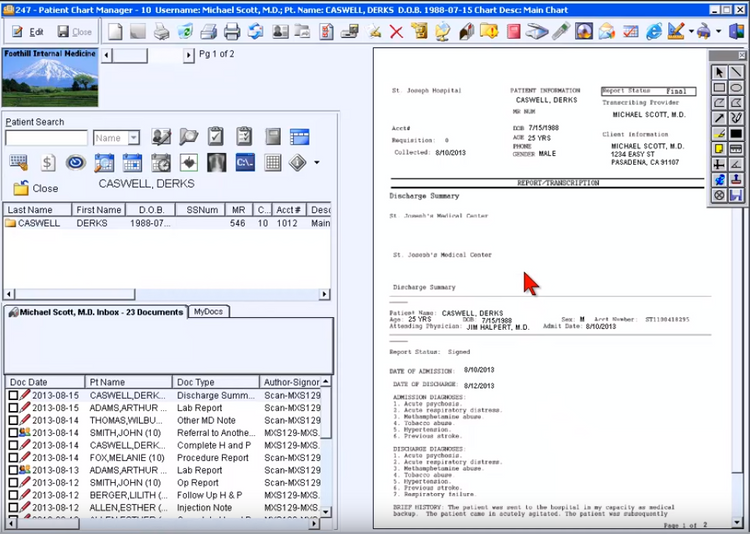
The Best Medical Billing Software
Get the best software for your business. Compare product reviews, pricing below.
What is Medical Billing Software?
Medical billing software is a highly-specialized accounting solution for generating and submitting payment invoices to patients and their health insurance companies. These invoices, known as claims, use special HIPAA-compliant codes to indicate different procedures, diagnostics, and medications provided to the patient. Each code is then run through the software to determine the total price of the patient’s bill. Healthcare facilities from single-doctor practices to hospitals all rely on medical billing software to accurately generate claims and collect payments.
Claims are usually sent either directly to the patient or to their insurer (the payer). In some situations the claim will first go to an organization like Medicare or Medicaid. Medical billing software allows you to send the initial claim to the correct payer for processing.
Medical billing software differs from hospital management software because it’s designed for the unique third-party payment problems of the healthcare industry. This solution makes it easy for your front office to address HIPAA-compliance, copays, insurance companies, and collection agencies.
Medical Billing Software Features
- Electronic Claim Generation: Create and submit electronic patient statements and claims to health insurance companies.
- Claims Processing: Track active claims and process incoming payments automatically.
- Collections Follow-Up and Reminders: Receive timely updates whenever a claim moves to collections or needs follow-up on your end. Remain in contact with collection agencies as they try to collect payment.
- Automated Recurring Charges: Bill long-term and repeated care services on a monthly or weekly basis.
- Payment Posting: Once a patient or insurance company has paid a claim you’ll know about it. Accurately update accounts receivable to keep your general ledger balanced. Send electronic remittance advice in a timely manner based on payment date.
- Self-Pay Patient Portals: Promote patient engagement by allowing direct access to account information online in order to make payments. Securely process credit card payments or money transfer from banks.
- Basic Accounting: Use a general ledger (GL) to track A/R patient and insurance charges.
- Code Engine: Current database of popular billing codes like: DRGs, HCCs, APC, ASC, NDCs, GPIs, ICD-9, ICD-10, CPT, and HCPCS. These codes are automatically updated over time to better reflect patient data.
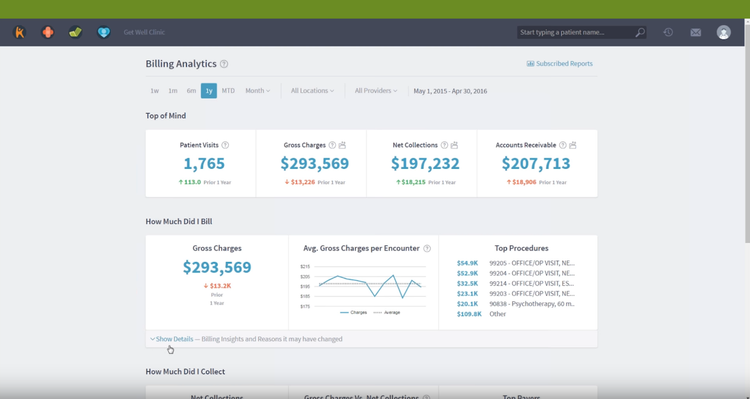
Benefits of Medical Billing Software
Medical billing software has many benefits for healthcare centers:
Revenue Cycle Management for Streamlined Payments
Healthcare practice management is hard enough without having to juggling late or missing patient payments. If your billing system isn’t managed online you’re making more work for yourself. One way to improve your medical billing is to use a Revenue Cycle Management (RCM) module to automate payment processing.
RCM solutions track all patient interactions in the billing process from appointments to final payment. You can provide better patient care by keeping accurate records of their medical bills. You’ll have the ability to follow-up on their insurance claim submissions and denial management if necessary.
When there are medical disasters, like a pandemic, manually tracking patient payments on paper may lead to a lot of mistakes. Use an RCM tool to stay on top of invoices and payments even when dealing with an influx of patients.
HIPAA Compliant Payment Processing
Medical billing codes were created, in part, to make it easier to distribute patient information without sharing their personal, private medical records to third-party organizations. By using codes, a billing solution only shares a price with clearinghouses, insurance companies and collection agencies.
Medical codes keep the electronic health records (EHR) of patients secure. Make sure to use HIPAA compliant accounting software to manage the rest of your healthcare finances. This includes sending electronic remittance advice to confirm patient or insurance payment.
In-House Medical Bill Scrubbing Saves Money
Healthcare clearinghouses check over medical claims from the biller before they are sent to patients or insurance companies. Their job is to ensure each claim is free from common errors like upcoding by “scrubbing” the invoice. Once clear, the claim is then submitted to insurers in a compatible format.
If any errors are found by the insurance company the claim submission may be denied or rejected. You’ll have to submit a new, corrected claim if you want to get paid. Scrubbed claims cut down on the amount of times a claim might be rejected by insurers.
If your healthcare facility wants to avoid using a clearinghouse, consider using a medical billing software to scrub your claims yourself. Cutting out the clearinghouse can save you time and lower your operating costs as claims go directly to patients and insurers. Integrate your billing solution with a hospital accounting software to cover all your finances.
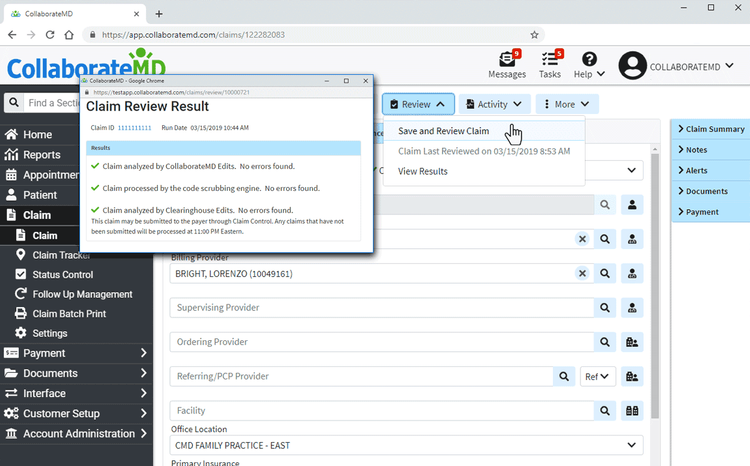
Instant Account Access Anywhere
Need to check a claim status while out of the office? Meeting with an insurance company to discuss a rejected claim? Mobile medical billing software lets you access information anywhere you go. You can get real-time updates on claims and collections before making any changes to a patient file.
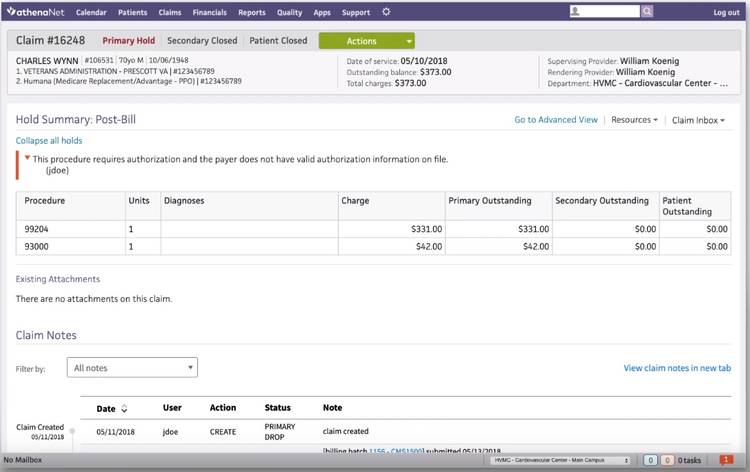
Medical Billing Codes
Different billing codes are used to indicate what condition a patient was diagnosed with, what treatments they received, where they were treated, and any medications they were prescribed. Every code has a cost associated with it.
The main types of medical billing codes are:
- Diagnostic codes: These codes classify the disease, injury, or disorder diagnosed by a medical professional. The most popular diagnostic codes are ICD-9-CM and ICD-10 including ICD-10-CM.
- Procedural codes: These codes refer to specific medical practices used during appointments. This can range from in-office procedures to surgical interventions. The main examples are CPT, HCPCS, ICPM, and ICHI
- Pharmaceutical codes: These are the codes which correlate to a specific medication, either by type or brand. Commonly used pharma codes are ATC and NDC.
- Topographical codes: These codes indicate the specific spot on the body treated or diagnosed. ICD-O and SNOMED are the main types of topographical codes.
Medical billing software is designed to keep all these different types of codes organized so doctors, nurses, and other staff can accurately charge patients for services.
Pain Points of Medical Billing
While medical billing is supposed to make healthcare easier to afford, there are a few problems:
Dealing with Insurance Companies
Insurance billing isn’t easy. Insurers want to avoid making large reimbursement payouts to patients and their healthcare providers. They’ll look for any error in a medical claim in order to outright reject it. By using medical billing software you have the chance to scrub every claim for errors before submittal.
Medical codes can be super specific to streamline the submission and acceptance process. There are already codes for injury from spacecraft collisions! Use billing software to make your patient claims as precise as possible to increase acceptance rates from insurers.
Dealing with Patients
Patients don’t know a lot about medical billing codes. If they don’t understand something on their bill, they’re likely to question the final price. For example, a patient who was diagnosed with the common cold might not know what “J00 acute nasopharyngitis” means on their bill. They might assume the bill was sent in error and refuse to pay. Accurate coding helps patients understand their electronic medical records (EMR).
Electronic billing also cuts down on the time between patient treatment and claim submission. Instead of receiving a bill months after receiving a service, the turnaround time can be narrowed down to days or weeks. Patients are more likely to dispute a charge if they can no longer remember the details of their appointment. The faster your medical billing service, the likelier patients are to pay.
Dealing with Medical Staff
Finally, your healthcare workers can be the source of the problem. Data entry errors are very common, especially during long shifts. All it takes is typing a 0 instead of a 9 to wind up with an incorrect claim that’ll be rejected by insurance. Scrubbing applications check over codes before they’re sent, helping doctors, nurses, and administrative staff catch errors early. And an electronic billing service stores patient records automatically for simple review whenever you need it.